Dr. Bahar Esmaili says that since posture can affect breathing, clinicians should utilize postural assessment as an objective screening measure.
 by Dr. Bahar Esmaili
by Dr. Bahar Esmaili
Humans express their full developmental and structural potential by epigenetic influences such as the mastication of hard, fibrous foods and walking barefoot on soft, uneven ground. Post-industrial life is mostly devoid of these triggers. Humans live with unexpressed potential for ideal development and instead are subjected to factors which trigger compensatory responses of one form or another along the kinetic chain. For example, walking on hard, level surfaces instead of uneven surfaces and grass is an ascending issue which can negatively affect the arches of the feet and how the spine is aligned over the hip. This is observed in exaggerated spinal curvature: Hyper-lordosis in lumbar spine leads to unstable hip posture, and kyphosis in cervical spine limits the ribcage expansion necessary for proper diaphragmatic and nasal breathing.
The human kinetic chain is a closed loop of ligaments, fascia, bones and fluid, with two hard boundaries: the ground as the contact point of the feet and the occlusal surfaces of the teeth as they come in contact. Any compensation between these two boundaries is manifested in and along one or more of the systems which comprise the kinetic chain. Anatomy and compensation determine static and dynamic posture. Posture is a profoundly simple yet reliable reflection and indication of the Autonomic Nervous System (ANS) at work to overcome obstacles which interfere with and even prevent normal bodily functions, including breathing and balance.
The Autonomic Nervous System controls the position of the mandible in relation to the maxilla (inter-arch relationship), cervical spine (parapharyngeal space), cranium (TMJ), and the hyoid bone (tongue posture) through several innate reflexes. Mandibular positioning to facilitate optimum nasal flow, from the ala of the nose to the epiglottis, can be determined using these reflexes: Breathing; Maintaining the Balance of the eyes with the horizon; and Keeping the Brain over the center of gravity during static posture and gait. This is the core principle of the Rule of the 3B’s: Breathe, Balance, and Brain.
Conversely, a top-down or ‘descending issue’ originates from blocked nasal passages and a soft diet. Children reared in post-industrial households are subjected to poor air quality and highly processed, genetically modified foods, resulting in chronic and systemic inflammation. Such inflammation leads to hormonal imbalances which result in enlarged turbinates and dysregulated nasal cycling, restricting nasal passages. Resultant mouth breathing deprives the body of many vital functions of the nose, including warming, humidification, and filtration of the air, supply of Nitric Oxide, and neural signals to the brain of speed and flow of air. Moreover, blocked nasal passages lead to low tongue posture and dysfunctional swallowing, which negatively impacts facial growth and aesthetics. Soft diets, requiring less functionally-directed growth and swallowing patterns, contribute to these compromises as the body must compensate.
Both ascending and descending culprits create compensatory muscle recruitment patterns in walking, standing, breathing, swallowing, and chewing. As such, patients with these patterns of compromise can rightly be said to be ‘financing the airway with poor posture.’ This is the beginning of a domino effect that disrupts the eruption of the teeth, interferes with the correct neurosensory pattern (garbage in, garbage out), and shows itself in malocclusions such as excess overbite and overjet, underbite, and crossbite. Malocclusion creates avoidance patterns and negative feedback loops that slow or even arrest normal growth and development. Additionally, crossbite prevents free and unimpeded latero-trusive motion of the lower jaw. Inhibition of normal range of motion of the mandible emerges as an additional postural issue, as the neck goes into forward translation during gait, motion and swallowing. These and other positive and negative feedback loops lend ongoing support to the oft-quoted observation of architect Frank Lloyd Wright: Regardless of whether one is referring to buildings or bodies, Form Follows Function, and Dysfunction leads to Deformity.
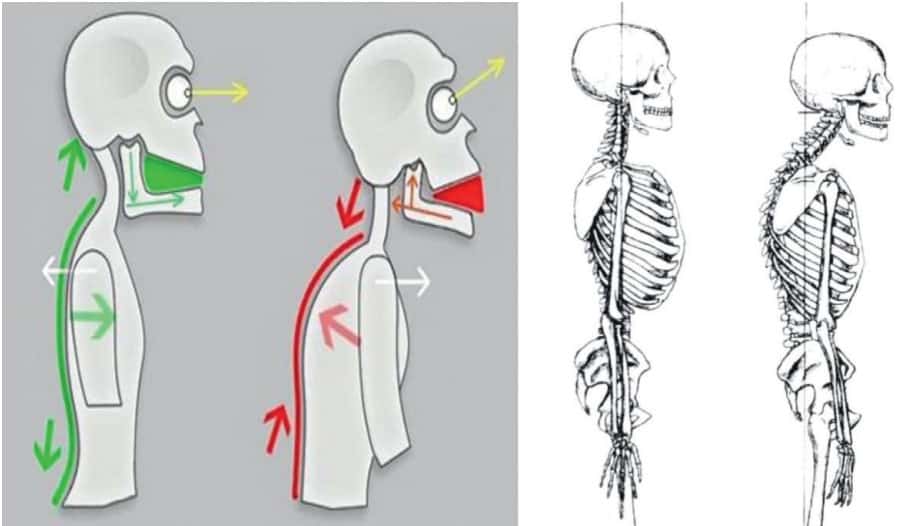 The mandible is an integral component of posture which is itself expressed by the functionality of the kinetic chain, influencing the position of the head over the spine as well as the alignment of the cervical spine in order to support the weight of the head over the center of gravity. As a consequence, the mandible moves in the opposite direction of the head, very often resulting in postural distortion. When the head assumes a forward posture (anteriorization and extension) as a compensatory breathing mechanism, the mandible moves in the opposite direction to guide body mass to support the head, and this in turn results in excessive overjet. During growth and development, the distalized mandible leads to impaired condylar growth and collapsed vertical dimension of occlusion (increased overbite), negatively impacting the retroglossal portion of the airway and cervical spine alignment.
The mandible is an integral component of posture which is itself expressed by the functionality of the kinetic chain, influencing the position of the head over the spine as well as the alignment of the cervical spine in order to support the weight of the head over the center of gravity. As a consequence, the mandible moves in the opposite direction of the head, very often resulting in postural distortion. When the head assumes a forward posture (anteriorization and extension) as a compensatory breathing mechanism, the mandible moves in the opposite direction to guide body mass to support the head, and this in turn results in excessive overjet. During growth and development, the distalized mandible leads to impaired condylar growth and collapsed vertical dimension of occlusion (increased overbite), negatively impacting the retroglossal portion of the airway and cervical spine alignment.
Patients compromise by ‘financing the airway with poor posture.’
Obstruction of the nasal airway at any point from the nasal valve to the base of the tongue will trigger an upregulation of the sympathetic branch of the ANS in order to negate the limitation of air flow. Forward head posture to clear the airway leads to spinal curvature and postural imbalance which is a secondary source of stress on the spine, in turn keeping the ANS in high sympathetic tone to execute functions as simple as sitting, walking and breathing. Clinicians can utilize postural assessment as a simple, no-cost, non-invasive and objective screening measure effective at assessing the sympathetic activity. Together with simple nasal flow screening, effects on the human kinetic chain can be demonstrated to both the clinician and to the affected person.
The first line of diagnosis should start with a head-to-toe examination of the patient to identify ascending and descending issues. Be curious about the level and degree of compensatory mechanisms, keeping the Rule of 3B’s in mind.
The order of inquiry is as follows:
- Can the patient breathe through the nose?
- Does the architecture of the airway including maxillary shape and position, nasal passage size and tissue health, and the posture of the tongue and palate allow unrestricted airflow?
- Can the diaphragm fully relax and contract?
- Is the hip neutral?
- Is the rib cage able to expand without restriction?
- Does spine have the normal curvature in all segments?
- Is the head over the spine or in front of it?
If you are wondering whether you have the clinical expertise to ask these questions, congratulations! You are a curious clinician, a lifelong learner. Master the meaning behind these questions and enjoy helping your patients to even better health.
Dr. Shad Morris talks about posture during sleep — read his article on positional therapy here: https://dentalsleeppractice.com/positional_therapy/.

 Dr. Bahar Esmaili grew up in Iran and immigrated to the United States when she was 20 years old to persue her dream of becoming a doctor. Since graduating with honors from the University of Colorado School of Dental Medicine in 2009, she has completed numerous advanced Continuing Education courses in the fields of craniofacial pain, TMJ disorder, and airway dentistry, and currently focuses her clinical practice on the connection between oral and whole-body health. She holds the prestigious position of being one of 24 North American consultants with 3M as part of the Council of Innovative Dentistry. She is a passionate educator and goes out of her way to help her patients understand the ‘why’ behind the ‘what’ of the issues for which they’re seeking help. She is a certified personal trainer, specializing in corrective posture and is passionate about the interconnectedness of the human body – from head & neck posture to jaw joint alignment to facial muscle tonicity to gait. In light of her profound realization that straight teeth cannot fit on crooked bodies, she is on a mission to enlighten practitioners of their ability to impact compensatory mechanisms that ultimately lead to the breakdown of our bodies and our health. She is excited to launch Project Compensation Nation and to inspire patients and professionals alike.
Dr. Bahar Esmaili grew up in Iran and immigrated to the United States when she was 20 years old to persue her dream of becoming a doctor. Since graduating with honors from the University of Colorado School of Dental Medicine in 2009, she has completed numerous advanced Continuing Education courses in the fields of craniofacial pain, TMJ disorder, and airway dentistry, and currently focuses her clinical practice on the connection between oral and whole-body health. She holds the prestigious position of being one of 24 North American consultants with 3M as part of the Council of Innovative Dentistry. She is a passionate educator and goes out of her way to help her patients understand the ‘why’ behind the ‘what’ of the issues for which they’re seeking help. She is a certified personal trainer, specializing in corrective posture and is passionate about the interconnectedness of the human body – from head & neck posture to jaw joint alignment to facial muscle tonicity to gait. In light of her profound realization that straight teeth cannot fit on crooked bodies, she is on a mission to enlighten practitioners of their ability to impact compensatory mechanisms that ultimately lead to the breakdown of our bodies and our health. She is excited to launch Project Compensation Nation and to inspire patients and professionals alike.