As “oral physicians”, we have an opportunity and obligation to reach across the aisle to our medical colleagues and collaboratively address systemic health issues. Looking past the teeth, gums and temporomandibular joints, we can observe the patient more comprehensively and use the oral cavity as an important health indicator. In the words of one of the founding father of Johns Hopkins Hospital, Sir William Osler, “The good physician treats the disease; the great physician treats the patient who has the disease.” Osler called the oral cavity a mirror of the rest of the body.1 As a hospital-trained dentist and medical school faculty, I have learned, taught and crossed the aisle with this discipline. The field of sleep medicine has provided a platform for a unique collaboration between dentists and sleep physicians.
The diagnosis and treatment of sleep disturbed breathing typically resides within medicine. This most often results in a CPAP (continuous positive airway pressure) solution. The attractiveness of CPAP’s 100% efficacy can blind providers to the poor compliance and compromised MDA (mean disease alleviation)2. The dental team, led by “oral physicians”, however, has the best vantage point for screening and recognizing the anatomical variants, phenotypic expressions, and other patient centric circumstances as contributors to successful treatment. This collaborative dialogue could further improve the effectiveness of treatment modalities that are available. Individualizing treatment and matching appliance type and design features, improves the efficacy, efficiency and ultimately the effectiveness of treatment.
ProSomnus Appliance
Typical CPAP Machine
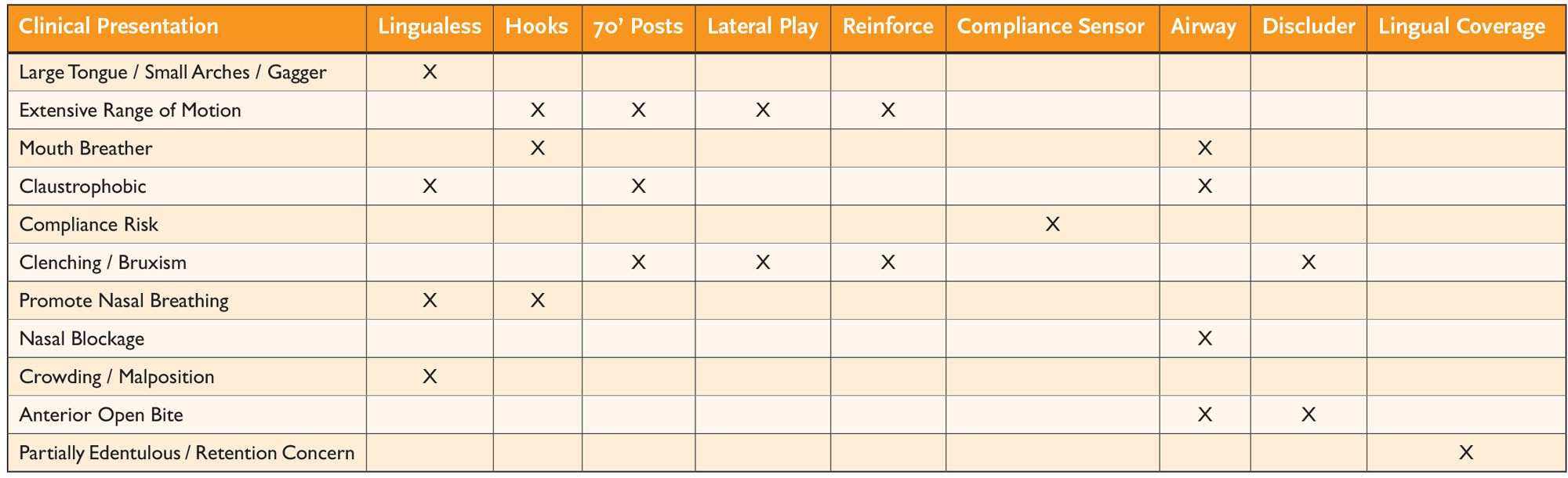
Imagine the following: During a routine dental visit, the dentist identifies a patient at risk for sleep related breathing disorder who also reports history of chronic sinus congestion, hypertension, lightheadedness and occasional episodes of skip beats in his pulse. The dentist initiates a referral to a sleep physician colleague for further testing and diagnosis, emphasizing the potential associated comorbidities. The sleep specialist, using this screening results as a jumping off point, orders a sleep test and determines the patient has a sleep disorder which could also be contributing to the other reported health concerns. The patient does not qualify for the standard CPAP therapy, due to the chronic sinus congestion and therefore receives a prescription for oral appliance therapy. The sleep specialist refers this patient back to the dentist for oral appliance fabrication with design specification to include advantages for their chronic sinus congestion. In this scenario, the dentist not only initiated an impressive preliminary screening observation for a sleep related problem, but also made a point of the associated comorbidities to the referring physician. The subsequent prescription for an oral appliance provided an opportunity for the dentist to customize the choice, design and therapy to meet the patient’s expression and condition, because, one size or design does not fit all. The ProSomnus [IA] device has a myriad of features that can be applied to offset anatomical variations, circumstances, and phenotype expressions that a patient may present with. The chart above shows some of the Monogram features available and the clinical presentations they support.
There are many oral sleep appliance manufacturers, but few have been able to be as responsive to the rate of change in medical science and have the necessary platform to accommodate design features addressing discoveries as they are made in the field of sleep medicine as ProSomnus Sleep Technologies. Their proprietary, patented system allows for the precise digital fabrication of a customizable device, which drives improved patient compliance, efficacy, efficiency and outcomes3,4.
The future is undoubtedly bright, exciting and rewarding. Through new technology, proven science and acceptance of multidisciplinary collaboration among experts in the field such as sleep medicine, the odds of success will inevitably rise, as new opportunities for collaborations are already here and gaining traction.