
By Ronald S. Prehn, ThM, DDS
 Patient: Matthew is a 17-yr. old male with OSA and CPAP intolerant due to Cerebral Palsy (CP). He is a special kid who is full of happiness and brings joy to others.
Patient: Matthew is a 17-yr. old male with OSA and CPAP intolerant due to Cerebral Palsy (CP). He is a special kid who is full of happiness and brings joy to others.
Diagnosis: OSA. AHI 14; RDI 15; PSO2 89%; 6 central apneas
Previous Treatment: CPAP was attempted, but with his CP he was not able to keep his head from moving and keep the mask on his face. Also, his mouth is wide open most of the night. Was referred by Texas Children’s Hospital for consideration of Oral Appliance Therapy.
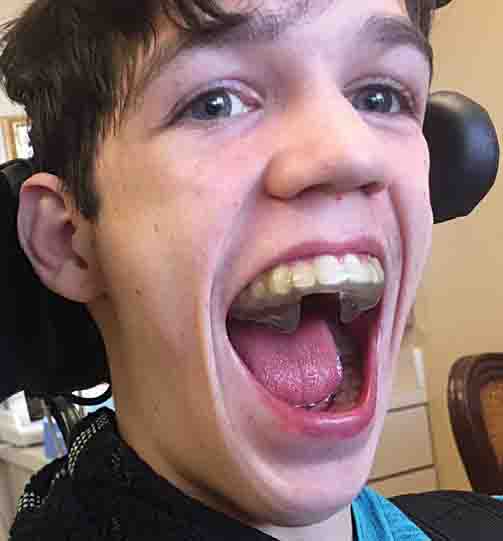
History: Matt had a history of facial pain, TMJ and jaw pain, morning HA, tooth pain from severe clenching, bruxing, insomnia, moderate snoring and fatigue. His mother and father said that since he was a child, he has woken up every 2 hours during the night, and so were they. They switch nights watching over him. Epworth Sleepiness Scale was 15. CPAP was attempted, but after trying multiple masks, he was unable to keep them on his head.
Exam: He had previous orthodontics 3 years ago, and his bite was class 1 at the time (per parents). Today he presented as a new patient with a 5mm anterior open and a 10mm over jet, due to severe tongue thrust. Oral exam was difficult due to his movement, but he had all his permanent teeth with good periodontal health. We were able to obtain a cone beam x-ray that showed he had no significant tonsils, and average size airway and a severe high vaulted palate. TM joints were well formed and free of arthritis. Images also confirmed his anterior open bite and over jet that started at the canines.

Treatment Considerations: The parents main concern about an oral appliance (OA) for sleep, was that with Matt being a quadriplegic, he would not be able to remove it himself. I had two concerns in trying to advance his mandible with any Mandibular Advancement Splint (MAS). First was that his mouth would be too open most of the time. The second was his severe clenching during certain periods at night. I did not think any MAS could control his mouth and stay retained on the teeth, or if a side winged MAS was used, he would over open to disengage the wings or break them off.
Treatment: With my background in Orofacial pain, I remembered the anterior repositioning splints that were used in the 1980s to treat TMJ. With our new understanding that bruxing is possibly a compensatory mechanism to protect the airway, I thought that this anterior repositioner worked at the time, because every time the patient clenched to protect the airway, the splint would advance the mandible and the clenching would stop because the airway opened. So, I took that idea and decided to fabricate a single arch upper anterior repositioning splint to advance his mandible 5mm when he clenched. If that mechanism of action were accurate, then this splint should resolve his OSA.
Result: At the one week follow-up, the mother (who was skeptical) came in with Matt crying. She said for the first time in 18 years, he slept through the night. She kept waking up checking on him to see if he was breathing! HST demonstrated resolution as his ODI was 4 events an hour and his PSO2 was 90%. All symptoms resolved.
If that mechanism of action were accurate, then this splint should resolve his OSA.
Discussion: Using our assertion that clenching is a protective mechanism for a collapsing airway, we were able to use an anterior repositioning TMJ splint that advances his mandible only when he clenched. While not ideal, it was enough airway support to maintain his airway and reduced the arousals to the point that he had resolution of symptoms. This treatment should be considered when faced with the challenges that Matt brought to this sleep clinic. Words cannot express the feeling of relief on the parents face when they returned for follow up. Matt had a friend recently pass due to his OSA. And now their son will be better able to face the challenges of CP in his day to day life, without the fatigue, the facial pain and without the fear of dying.
