
by Michael Flanell, RDH, MBA
Athletes continually try to perform better and break records with their athletic abilities. In their pursuit for personal accomplishments, they dream of winning medals for themselves, their teams, and their countries as well as becoming part of professional organizations. What if small changes in how an athlete breathes could support greater athletic performance? Learning to breathe properly may, in fact, make the difference between winning and losing.
In athletic competitions, astute observers will notice that some athletes breathe through their mouths, while others breathe through their noses. I urge you to pay attention to this next time you watch a sporting event. Could this matter in an athlete’s ability to win? Roger Federer, aged 37, ranked number three in men’s singles in 2018 by the Association of Tennis Professionals, and Federer’s mouth is almost always closed during competitions. Nasal breathing presents physiological advantages that are particularly helpful to competitive athletes, and athletes should be trained to breathe through their noses whenever possible.
Respiration is a fundamental physiological process and finding the most efficient breathing mode during exercise warrants further exploration. Breathing, or ventilation, is the process of gas exchange from the outside environment to the alveoli. For optimal athletic performance, the goal is to utilize oxygen (O2) as efficiently as possible. The greatest athletes in the world are able to consume more O2 in their muscles while keeping carbon dioxide (CO2) levels low.1
Mouth breathing syndrome (MBS) is characterized by inhaling and exhaling primarily through the mouth and is considered to be an abnormal respiratory function. According to Capitanio de Souza,2 MBS is a pathology that is associated with the obstruction of the upper airways and increased resistance of nasal breathing. MBS can be induced by factors such as tonsil hyperplasia, hypertrophic turbinates, rhinitis, tumors, infections, inflammatory disease, and abnormalities in nasal architecture. Another cause of MBS is improperly developed orofacial muscles from infancy due to factors such as bottle feeding, finger sucking and/or nonnutritive sucking, making those muscles more flaccid and hypotonic.3 Prolonged mouth breathing can lead to muscular and postural alterations, which may cause dentoskeletal changes.4 Consequently, the habit of breathing through the mouth, even without obstruction, alters the balance of facial muscles and causes facial skeletal changes.
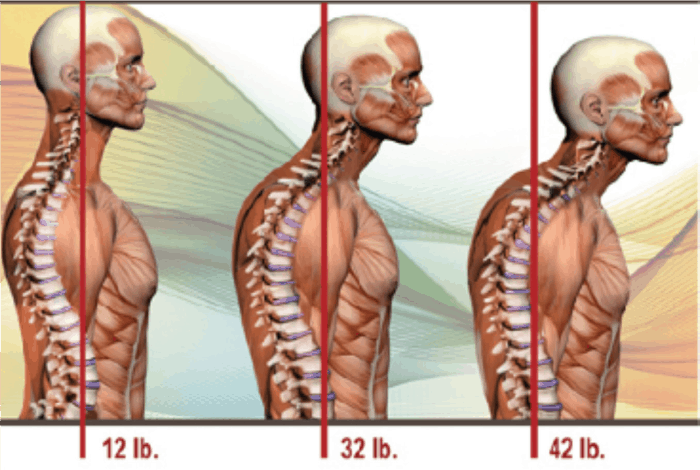
Many healthcare professionals are unaware of the negative effects of MBS and that MBS can lead to changes in tongue and head position. With MBS, the location of tongue is down and backwards instead of up and forward in the palate. The tongue position influences the palatal development and, if not properly positioned in the palate, can result in a deep vaulted hard palate and a deviated septum contributing to MBS, instead of a domed formation and properly formed septum. The tongue resting in the lower jaw can cause a forward head position. Every inch of forward head posture increases the weight of the head on the spine by approximately 10 pounds5 creating an adverse load on the cervical joints, induced by poor spinal, cervical, and scapular postures. Additionally, the forward head position may strain the deep postural-stabilizing muscles of the spine, reducing the performance of their functional postural-supporting role.6
A significant problem with MBS is the reduction of oxygen absorption leading to a downward spiraling effect on sleep, stamina, and energy levels, all vital to the athlete. This effect is caused by inhaling too much oxygen and exhaling large amounts of carbon dioxide, needed for the transfer of oxygen from the hemoglobin molecule during respiration in the lungs. Breathing through the mouth also causes dryness of the oral and pharyngeal tissues and may lead to inflamed tonsils, tonsil stones, dry cough, swollen tongue, halitosis, and gingivitis. Mouth breathers also chew with their mouths open and swallow air, leading to gas, bloating, flatulence, and burping. In addition, lips become dry and flaccid because they do not stay closed to provide the necessary lip seal.7
Mouth breathing causes biochemical, physiological, and immunological disturbances. Among the biochemical and physiological disorders related to MBS are lower oxygen absorption (chronic hypoxemia), increased CO2 concentration (hypercapnia), and changes in the acid-base balance, towards respiratory acidosis. Mouth breathing is also associated with increased water loss, decreased energy, and changes in salivary profile resulting in a greater risk of heat stress and disrupted muscle function, thus negatively affecting athletic performance due to dehydration. According to Garcia Triana,8 healthy subjects experienced a 42% decrease in net water loss when they switched their breathing mode from nasal to oral expiration during tidal breathing.
Additionally, mouth breathing can cause changes in sleep patterns, which can contribute to a decrease in immune defense cells and an increase in humoral serum values related to inflammatory mediators, indicating the occurrence of oxidative stress and an altered systemic inflammatory state. Considering the athlete as a patient, a reduction in the quality or quantity of sleep can result in biological and cognitive imbalance, potentially decreasing physical performance and the recovery process after a workout.2 In addition, the decrease in immune defenses cells puts the athlete at risk for contracting illnesses, which may compromise performance during the athletic event.
The nose has numerous functions: olfaction, sensation, mucociliary clearance, filtration, and immunological functions. In addition, the nose has the function of regulating air from cold to warm and humidifying the air during the nasal cycles of airflow dynamics. Nasal breathing cleans the air as it enters the body, produces nitric oxide (NO), and performs the same amount of work with less energy expended. Immunological functions of the nose produce mucus and secrete immunoglobulins. The nose has its own self-defense due to its coarse hairs (vibrissae) and the secretions it creates. In addition, the nose protects the lungs from allergens, toxicants, and other bacteria through its immunologic properties. Mucociliary clearance promotes mucus and cilia functions: to filter and trap toxicants and transport airborne particles.9 According to Lacomb, humidification occurs within 80% of the air before it reaches the lungs. Air is heated through conduction, convection, and radiation with blood flow in the opposite direction to incoming airflow, allowing for greater efficiency in warming the air.
As ambient oxygen (O2) passes through the sinuses, it diffuses across the nasal epithelium and can be used by the cells to produce NO. As the sinuses produces NO and air is continuously inhaled, NO reaches the lungs and is diffused into the capillaries of the surrounding alveoli, expanding vessels and increasing O2/CO2 exchange.
Lundberg,10 noted that the release of NO helps to control blood flow via diffusion to the underlying smooth muscles cells. The powerful vasodilating effects of NO lead to increased oxygen uptake, a reduction in pulmonary vascular resistance, and arterial oxygenation.
 The benefits of enhanced NO productivity include increased aerobic capacity, reduced hypertension, increased insulin sensitivity and glucose tolerance, capillarization and angiogenesis, and even long-term potentiation (LTP) associated with cellular models for learning and memory.11 An additional benefit of enhanced NO productivity is neurogenesis, which is the process by which new neurons form in the brain. These physiological conditions can either positively influence an athlete’s performance or impair the outcome. Nitric oxide, through nasal breathing, regulates autonomic functions like heart rate, respiration, blood pressure, and digestion along with mood, sleep cycle, fluid balance, and reproduction.11 The increase of blood flow derived from NO synthesis may improve recovery processes as well. According to Lacomb, nasal breathing, due, in part, to increased flow rates of air throughout the lungs, reduces exercise-induced asthma and bronchoconstriction.
The benefits of enhanced NO productivity include increased aerobic capacity, reduced hypertension, increased insulin sensitivity and glucose tolerance, capillarization and angiogenesis, and even long-term potentiation (LTP) associated with cellular models for learning and memory.11 An additional benefit of enhanced NO productivity is neurogenesis, which is the process by which new neurons form in the brain. These physiological conditions can either positively influence an athlete’s performance or impair the outcome. Nitric oxide, through nasal breathing, regulates autonomic functions like heart rate, respiration, blood pressure, and digestion along with mood, sleep cycle, fluid balance, and reproduction.11 The increase of blood flow derived from NO synthesis may improve recovery processes as well. According to Lacomb, nasal breathing, due, in part, to increased flow rates of air throughout the lungs, reduces exercise-induced asthma and bronchoconstriction.
As demands of physical activity increase, athletes may switch from breathing nasally to oronasally, or to breathing completely orally. There is, however, no exact switching point, due to a wide variance in people’s breathing patterns and needs. Ninnima12 found that the size of the nasal airway was the greatest contributor to switching, and, in addition, the larger the nasal airway, the longer the individual was able to breathe through the nose. Athletic performance can, however, be inhibited by nasal breathing at the point when exertion becomes more intense. Oral breathing occurs in shallow, quick breaths in order to receive more oxygen (O2) into the lungs and higher carbon dioxide (CO2) into the body.13 At higher intensities of physical activity, nasal breathing cannot provide the volume of O2 that oral breathing can, and less O2 content will result in a decrease in athletic performance. On the other hand, while mouth breathing at high levels of exertions may result in hyperventilation, nasal breathing effectively reduces this state. The evidence, thus, still supports nasal breathing, even at higher levels of performance, as a more efficient mode, given that the same amount of mechanical work is completed at a lower metabolic cost compared with oral respiration. Using nasal expanders can, therefore, increase the capacity to sustain moderate to intense physical exertion during nasal breathing.8
In conclusion, nasal breathing provides significant advantages over mouth breathing, particularly for athletes who want to improve performance as well as recover more efficiently. The many benefits include a better night’s sleep in preparation for an event as well as managing input versus output with O2 and CO2 exchange. Nasal breathing releases NO, which regulates homeostasis in many of the body’s functions such as heart rate, blood pressure, and respiration. The disadvantages of MBS are the ill effects of poor posture from the tongue placement in the lower jaw, causing head-forward position as well as the inhalation of a larger than needed volume of dry, unfiltered air. Breathing through the mouth can also contribute to more dehydration in the athlete. Professional athletes who seek to maximize performance through breathing may want to include breathing coaches on their teams.
