CE Expiration Date: May 28, 2024
CEU (Continuing Education Unit):2 Credit(s)
AGD Code: 730
Educational Overview
In 2020, the American Academy of Dental Sleep Medicine published their position paper on dentistry’s role in home sleep testing (HST). This statement was a welcome advancement for dental sleep practices as part of a multi-disciplinary solution to the growing number of undiagnosed apneics in the United States.
In this self instructional course for dentists, Jagdeep Bijwadia, MD and Gregory Manning, DDS, describe the most common HST models employed by dental practices; their benefits and challenges, how the advent of telemedicine improves access to care for sleep patients, and what key criteria dentists should consider when evaluating a model that works for their practices.
Learning Objectives
Dental Sleep Practice subscribers can answer the CE questions online at dentalsleeppractice.com/continuing-education to earn 2 hours of CE from reading the article. Correctly answering the questions will exhibit the reader will:
- Understand the 3 most common home sleep testing models
- State the required number of channels for each type of HST
- Explain how telemedicine can facilitate HST in a dental sleep practice
- Determine an HST model that is appropriate for their practice
- Be familiar with various medico-dental professional organizations’ unique positions regarding HST and dentistry
In this CE, Drs. Jagdeep Bijwadia and Greg Manning discuss the roles of home sleep testing and telemedicine, and how they can improve access to care for sleep patients.
by Jagdeep Bijwadia, MD and Greg Manning, DDS
Data shared at the 2018 American Thoracic Society International Conference indicated sleep apnea prevalence to be just under 1 billion people worldwide.1 Home sleep testing (HST) is a disruptive technology that has changed the management of sleep apnea and reduced some of the barriers to care. While not appropriate for diagnosing many of the more complex sleep disorders, HST is safe, effective, and it provides valid data for the diagnosis of uncomplicated obstructive sleep apnea. Home sleep testing has improved access to care, expedited diagnostic pathways, and provided a wider reach to the population. This is particularly significant when one considers the roughly 80% of patients with sleep apnea who remain undiagnosed.2 The technology for testing continues to evolve with increased accuracy and reduced cost. There are several different ways dentists currently incorporate HST into their practices. Telemedicine allows dentists and physicians to collaborate in the care of the patients in real time further amplifying the power and ease of home sleep testing while meeting quality guidelines.

Background
In March 2016, the Centers for Medicare and Medicaid Services (CMS), whose reimbursement rules are generally adopted by private insurers, dropped its long-standing opposition to home studies.3 According to the National Coverage Determination that was released that month, a diagnosis of obstructive sleep apnea (OSA) could be made, and the cost of therapy covered on the basis of a clinical evaluation coupled with a home study. The guideline specified that the home study must be ordered and supervised by the treating physician. CMS also specified the types of HST devices that would be reimbursed.
CMS guidelines define 4 categories of sleep testing:
- Type 1: Attended studies performed with the oversight of a sleep technologist with full sleep staging and that must include the following channels. EEG, EOG, ECG/heart rate, chin EMG, limb EMG, respiratory effort at thorax and abdomen, airflow from nasal cannula and pulse oximetry, and additional channels to monitor CPAP, PH, CO2, et cetera.
- Type II: Home sleep test with type 2 monitor with a minimum of 7 channels that must include EEG, EOG, ECG/heart rate, EMG, airflow, respiratory effort and oxygen saturation.
- Type III: HST with Type III portable monitor, unattended with a minimum of 4 channels. Type III devices must include the following channels: 2 respiratory channels (flow and effort) ECG/heart rate and oxygen saturation.
- Type IV: A sleep testing device measuring three or more channels that include actigraphy, oximetry, and peripheral arterial tone is covered when used to aid the diagnosis of OSA in beneficiaries who have signs and symptoms indicative of OSA if performed unattended in or out of a sleep lab facility or attended in a sleep lab facility
The most commonly used home sleep tests are type III and type IV devices. In the next section we will review how these HST devices work and how the sensors are used to detect OSA.
Since Medicare’s adoption of HST, many private payors followed their lead. It is a truism that where payers go, clinicians follow and although the American Academy of Sleep Medicine (AASM) was initially opposed to the use of home sleep tests, it subsequently endorsed them with detailed guidelines for their clinical use.3
Polysomnography Versus Home Sleep Testing
Polysomnography (PSG) or an in-lab sleep test records numerous physiologic signals simultaneously during a patient’s sleep period. Signals recorded include EEG or brainwaves allowing sleep time to be directly accurately during the study period, airflow, abdominal and thoracic effort during breathing, as well as oximetry which allows diagnosis of various kinds of sleep disordered breathing (SDB). Electromyography of the chin and limbs is recorded. A video is recorded, and a trained sleep technician directly observes the sleeping patient.
Type 1 testing (PSG) can be used for the diagnosis of sleep apnea and many other complex sleep related breathing disorders like central apnea syndromes, hypoventilation, and Cheyne-Stokes respirations. The detailed physiologic data collected also allows diagnosis of several other sleep disorders like periodic limb movements, parasomnias, and nocturnal seizures. PSG can be combined with daytime sleep testing called multiple sleep latency testing to look for disorders such as narcolepsy and primary hypersomnia. Polysomnography is also used to initiate treatment with CPAP, BIPAP, or even oral appliances. This is called spilt night polysomnography. For all these reasons, PSG is often considered the gold standard sleep test.
Disadvantages of PSG include cost and the logistics of performing the complex testing. Since the patient is not in their own environment, natural sleep patterns may not be accurately reflected in the single night test. Additionally, significant backlogs can occur due to bed scarcity. PSG can be prohibitive in rural areas or geographical areas with an insufficient number of sleep clinics, too.
Given the high-cost burden, many insurance companies now require the clinician to specify why a polysomnography is needed and why a home sleep study is not sufficient. Specifically, when there is significant suspicion of OSA, most insurance companies will require an HST to be completed prior to authorizing an in-lab polysomnogram.
Type II portable monitors are unattended sleep studies that are performed without the oversight of a sleep technologist, with a minimum of 7 channels including EEG allowing for more accurate sleep time and sleep staging information.
As previously mentioned, the most widely used home sleep tests are type III and type IV tests. These HST devices typically record fewer signals that are specifically focused on the diagnosis of sleep apnea. For example, EEG signals are not available on Type 3 and 4 home sleep tests so sleep time is derived indirectly and is therefore less accurate. Additionally, as the name indicates, the study is done in the patient’s own home and there is no technician monitoring the patient. While HSTs have been extensively validated for the diagnosis of OSA and are extremely reliable, it is important to recognize that they are not useful for making diagnoses of more complex SDB. Home sleep tests are most useful when one is trying to confirm the diagnosis in a patient with whom you have a high clinical suspicion of OSA. It is important to recognize that home sleep tests are not very accurate in ruling out sleep apnea and a negative test in the setting of a high clinical suspicion for sleep apnea should prompt additional testing. The obvious advantages of HST are the lower cost and higher convenience. Newer, disposable HST units can be used multiple times, further reducing associated costs and increasing clinical usefulness. Since the tests are conducted in the patient’s home environment, they may more accurately reflect natural sleep patterns. Patients often express reluctance to undergo polysomnography but are generally more amenable to home sleep testing.
How Home Sleep Testing Works
Type 3 home sleep tests such as the Alice NightOne (Philips, The Netherlands) or the ApneaLink Air (Resmed, San Diego, CA) detect apneas and hypopneas through simultaneous analysis of airflow measured by a nasal cannula, effort measured by a respiratory impedance plethysmography belt, and an oximeter that detects changes in oxygen saturation. If airflow drops by 90% along with continued breathing effort, the event is identified as an obstructive apnea. If the airflow drops by at least 30% along with a 4% drop in oxygen saturation, then the event is detected as a hypopnea. By counting the number of apnea and hypopneas occurring every hour (called the apnea hypopnea index or AHI) the severity of sleep apnea is determined. Type 3 devices are also able to detect central apneas, occurring when there is an absence of airflow accompanied by absence of breathing effort. In addition to airflow, effort belts, and oximetry, many type 3 devices also offer actigraphy, heart rate, and body position monitors.
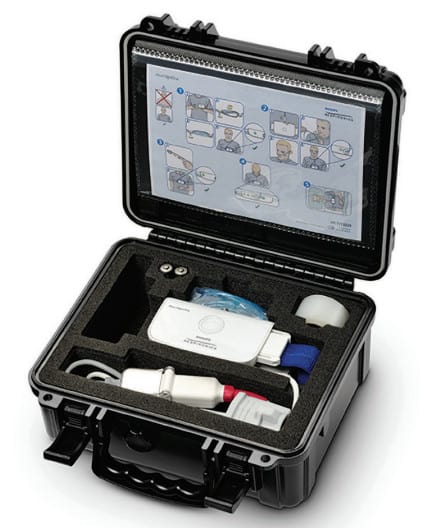
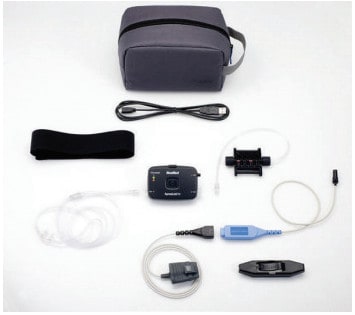

Type 4 home sleep tests such as the WatchPAT (Itamar Medical, Israel) and NightOwl (Ectosense Belgium) use alternate signals to assess the AHI. Numerous peer-reviewed studies have been conducted to confirm that the AHI calculated using these devices is comparable to polysomnography. With these devices, peripheral arterial tonometry (PAT) is used in combination with heart rate and oxygen saturation. When the airway narrows it causes a brain arousal which triggers arterial vasoconstriction causing the blood volume in a peripheral blood vessel such as in the finger to fall. This is usually accompanied by a rise in the pulse rate. Using different wavelengths of light and sophisticated algorithms, a sensor placed over a finger can detect the changes in peripheral blood volume as well as oxygen saturations. AHI is calculated by the simultaneous analysis of these signals. It is difficult to separate apneas from hypopneas with this technology and manual scoring is typically not performed as there are no published scoring guidelines for these signals.

Newer methods of assessing AHI include acoustic signal analysis of breathing patterns and snoring and ballistocardiography. Devices using this technology are commercially available but aren’t widespread clinical use. Nor are they reimbursed by payors, and further clinical validation is needed.

Traditional HSTs require initial investment in the device as well as some recurring disposable costs for each test. Additionally, there are logistics associated with deploying and monitoring the return of devices which adds some operational complexity for practitioners.
A significant recent advance has been the introduction of disposable HST devices. With the safety concerns brought forth by the Covid pandemic, adoption of disposable HST devices like the WatchPAT One (Itamar Medical, Israel) and the NightOwl has increased significantly. The patient pairs the disposable home sleep test device with a cell phone. Once the study is completed, the sleep test data is transmitted immediately via the cloud to a portal accessible to the interpreting physicians.

One feature which is especially useful for a dental sleep practice is the availability of disposable multi-night home sleep testing. The NightOwl provides not only the diagnostic testing but also several more nights of additional testing with the same small disposable device. This facilitates testing for multiple nights over several weeks as the dental device is titrated to its optimal position allowing objective assessment of treatment outcomes. While these devices have a higher per test cost, they have less upfront costs than other devices, and are now widely used.
Regulatory Issues and Professional Guidelines
To address the OSA epidemic, the American Dental Association weighed in with a policy statement in 2017.4 It stated that dentists are encouraged to screen patients for sleep related breathing disorders as part of a comprehensive medical and dental history to recognize symptoms such as sleepiness, choking, snoring or witnessed apneas and an evaluation of risk factors such as obesity, retrognathia or hypertension. These patients should be referred as needed to the appropriate physicians for proper diagnosis.
There is widespread agreement in the regulatory guidelines that sleep studies including home sleep tests must be interpreted by board-certified sleep physicians. There is however controversy surrounding who can order a home sleep test. The American Academy of Dental Sleep Medicine (AADSM) recently published a statement strongly in support of allowing dentists to order home sleep tests.5 The statement, co-authored by the AADSM president David Schwartz, DDS, D.ABDSM states, “It is within the scope of practice for a qualified dentist, defined by the American Dental Association (ADA) as a dentist treating sleep-related breathing disorders who continually updates his or her knowledge and training of dental sleep medicine with related continuing education, to order or administer home sleep apnea tests (HSATs).”
It is within the scope of practice for a qualified dentist, defined by the American Dental Association as a dentist treating sleep related breathing disorders who continually updates his or her knowledge and training of dental sleep medicine with related continuing education, to order or administer home sleep apnea tests.
Further cementing this position, Dr. Schwartz wrote in the Spring 2021 issue of Dental Sleep Practice, “This position statement makes it clear that the AADSM believes that:
- It is within the scope of practice for a qualified dentist to order or administer HSATs.
- Licensed medical providers should be diagnosing and verifying treatment”6
This statement is in stark contrast to the AASM’s position statement on the Clinical Use of a Home Sleep Apnea Test7 and the Clinical Practice Guideline for Diagnostic Testing for Adult Obstructive Sleep Apnea8 which clearly outline that a home sleep apnea test is used as a medical assessment, and its use must be preceded by a comprehensive sleep evaluation by a medical provider. This medical evaluation should include an assessment for chronic diseases and conditions that are associated with increased risk for obstructive sleep apnea, including hypertension, stroke, and congestive heart failure. An evaluation by a medical provider also is necessary to rule out conditions that place the patient at increased risk of central sleep apnea and other forms of non-obstructive sleep-disordered breathing. This medical evaluation is essential for identifying appropriate candidates for sleep testing and minimizing unnecessary tests.”
In the aforementioned Dental Sleep Practice editorial, Dr. Schwartz states his agreement with this ideal model but challenges its logistical capacity to meet the needs of the 54 million Americans who remain undiagnosed. He opined, “Would it be ideal for every patient in the country to have a face-to-face evaluation with a board-certified sleep medicine physician, have a polysomnogram, be presented with a variety of treatment options, get proper education on how to appropriately use their therapy, know who to contact when they have issues with their therapy and receive the appropriate follow-up care? Absolutely! And it’d be even better if all of this is done within seven to ten days.
But the reality is that this is impossible – for a bevy of reasons – for most of the 54 million Americans with sleep apnea. The American Academy of Sleep Medicine (AASM) has acknowledged that there are too few board-certified sleep medicine physicians; approximately 5,700 throughout the country, many of whom are in metropolitan areas and affiliated with academic institutions, to manage the obstructive sleep apnea patient population.”
The controversy centers mostly on whether ordering an HST is within the scope of dentistry. Standards for minimum training in dental sleep medicine and well-defined patient-centered collaborative practice protocols are needed and would go a long way to resolving some these ongoing discussions.
The American Academy of Sleep Medicine (AASM) has acknowledged that there are too few board-certified sleep medicine physicians; approximately 5,700 throughout the country…
Incorporating Home Sleep Testing into a Dental Practice
Due to these seemingly conflicting guidelines, incorporating home sleep testing into a dental practice can seem challenging. There are different approaches that a dental office can use. Each of these approaches present unique advantages and challenges.
Purchase a Home Sleep Testing Unit
A dental practice dispenses home sleep tests directly to patients while they are in the office. In most cases, the patient returns the unit to the practice the following day and the data from the sleep study is transmitted to a sleep physician for interpretation of the sleep study.
Estimated Time of Completion: < 1 week
It is important to note that a dental device is durable medical equipment and subject to Stark and anti-kickback laws.
Advantages:
- Higher patient acceptance as testing occurs at the same time as they are screened
- Revenue potential by charging patients for testing
- Decreased barrier to entry for patients as testing occurs with a trusted provider
- Tests are able to be dispensed by staff members and do not require the dentist’s direct contact
Challenges:
- Capital expenditure for HST units
- Recurring cost of disposables
- Risk associated with possible loss or damage to HST units
- Coordination of sleep physician interpretation
- Training team to dispense and maintain the units
Use a Home Sleep Testing Service
An option that’s seen exponential growth over the past few years involves 3rd party companies that manage home sleep testing for dentists. The dentist submits a prescription and necessary documentation for a home sleep test, and the company contacts the patient to ship a home sleep test to them. The service sends the test to the patient and upon the completing the test, the patient ships the test back to the company. These 3rd party services typically charge the patient a cash fee or works through their medical insurance and compensates their sleep physicians to interpret the sleep studies.
Estimated Time of Completion: 2-4 weeks
Readers should consider that once the studies are interpreted, the dentist must still to find a physician to write a prescription. If the dentist has a local physician who has seen the patient, and is amenable to writing the prescription, this model can work rather well.
Advantages:
- Eliminate upfront costs
- Avoid potential loss or damage of HST units
- Access to larger volume of HST inventory
- Reduce impact on dental staff time
- Increase patient acceptance compared to an in-lab polysomnography
Challenges:
- Patient non-compliance when company attempts to schedule test
- Reduced patient sense of urgency due to timeframe between screening and testing
- Loss of control in process and patients “falling through the cracks”
Refer to a Sleep Specialist
The dentist refers patients to a local sleep physician who can perform a face-to-face consult with the patient, order sleep testing, and prescribe treatment such as PAP or a dental device. Importantly, the sleep physician can address non-OSA related issues contributing to the patient’s symptoms.
Estimated Time of Completion: several weeks
Advantages:
- Minimal staff time required for referral to a sleep specialist
- Comprehensive testing and treatment coordinated by the sleep physician
- Meets all currently recommended practice guidelines for demonstrating patient-physician relationship and will return a prescription for therapy (when clinically appropriate)
- Fosters a collaborative relationship in which the sleep physician may refer future patients when oral appliances are indicated
Challenges:
- Possibility the sleep physician will order more expensive testing (polysomnogram)
- Extensive wait times for both consult and testing
- Many sleep physicians are skeptical of oral appliances and may order CPAP or alternative treatments
Key Considerations
When pondering an approach to home sleep testing, additional consideration should be given to criteria that doesn’t fit within the binary confines of the advantages and challenges juxtapositions covered thus far. A brief list of these considerations includes:
- State Dental Boards – A few states have limited the dentist’s scope of practice to explicitly prohibit ordering or dispensing HST. Verify your state board’s position prior to purchasing home sleep test units.
- Sleep studies interpreted by a sleep physician without a consult do not meet all currently recommended practice guidelines for demonstrating patient-physician relationship. A prescription for treatment requires a face-to-face evaluation with the provider prescribing treatment.
- Custom-fabricated oral appliances are classified as durable medical equipment and are subject to Stark and anti-kickback laws. Sleep physicians may have concerns with payment directly from a dentist to interpret sleep studies when there is an implicit expectation that the physician will write an oral appliance prescription for that same patient if clinically indicated.
- Most medical insurance companies mirror CMS guidelines and require that the HST and corresponding treatment are prescribed by a physician after an initial face-to-face consult with the patient.
Telemedicine and Home Sleep Testing
With the onset of the Covid pandemic there have been significant changes to the regulations governing the use of telemedicine. Telemedicine allows wide access to medical expertise without the risks of close contact both for patients and caregivers. Prior to the pandemic there were significant geographic barriers to using telemedicine. As an example, a physician could not see a patient via telemedicine unless the patient resided in a rural or underserved area. In response to the Covid pandemic, CMS made sweeping changes that allowed clinicians to use telemedicine across state lines and get reimbursed for the visits with the same payment scale as an in-person visit. Regulatory changes such as these have enabled dentists to refer patients to sleep physicians for telemedicine consultations as well as follow up on their own patients via these virtual platforms.
Most sleep physician offices now offer telemedicine consultations. Several third party HST companies including Awaken2Sleep, Better Night, SleepTest.com, and VirtuSleep offer integrated telehealth physician consultations as well.
In some models, physician online consultations are followed by a process of non-disposable HST devices mailed to the patients and results and prescriptions are communicated back to the dentists. The workflow is coordinated by the third party making the process easy and fairly seamless for the dentist.
Alternate models of care allow patients to leave the dentist’s office with a disposable HST. Online consultation with a physician is followed by test interpretation and dental device prescription in under two weeks. Additionally, the dentists can then use the same multi-night disposable HST to objectively optimize the dental device titration.
These are examples of extremely efficient, cost-effective workflows that meet all regulatory guidelines and encourage close collaboration between dentists and physicians across the entire OSA care pathway.
Final Thoughts
There is widespread recognition that obstructive sleep apnea remains underdiagnosed, and patients are seeking treatment option alternatives to CPAP. There is strong evidence that despite individual variability, dental devices can be highly effective in the right group of patients with mild, moderate, and even severe OSA. Dentists play a major role in identifying patients at risk and helping manage the epidemic of sleep disordered breathing. There are numerous home sleep testing models available to drive collaboration between physicians and dentists. Innovation and advances in technology are rapidly changing the way dental sleep medicine will be practiced in the future. Dentists should be on the front lines in this fight to impact the 80% of undiagnosed sleep apnea sufferers. Home sleep testing and telemedicine should be a part of a dental sleep practitioner’s armamentarium.
Read some insights on the legal aspects of home sleep testing from Jayme R. Matchinski, Esq. here: https://dentalsleeppractice.com/home-sleep-apnea-testing-and-dental-sleep-medicine/
References
- New Findings from University of California at San Diego Yields New Data on Sleep Apnea (Estimation of the global prevalence and burden of obstructive sleep apnoea: A literature-based analysis). (2019). Health & Medicine Week,
- Lee, Won, et al. “Epidemiology of Obstructive Sleep Apnea: a Population-Based Perspective.” Expert Review of Respiratory Medicine,S. National Library of Medicine, 1 June 2008, www.ncbi.nlm.nih.gov/pmc/articles/PMC2727690/.
- Kapur, Vishesh K et al. “Clinical Practice Guideline for Diagnostic Testing for Adult Obstructive Sleep Apnea: An American Academy of Sleep Medicine Clinical Practice Guideline.” Journal of clinical sleep medicine: JCSM: official publication of the American Academy of Sleep Medicine 13,3 479-504. 15 Mar. 2017, doi:10.5664/jcsm.6506
- Council on dental practice – dentistry’s role in sleep related breathing disorders. (2017, October). Retrieved April 10, 2021, from https://www.ada.org/en/member-center/leadership-governance/councils-commissions-and-committees/dentistry-role-in-sleep-related-breathing-disorders?utm_medium=VanityUrl
- Schwartz D, Levine M, Adame M, et al. American Academy of Dental Sleep Medicine position on the scope of practice for dentists ordering or administering home sleep apnea tests. J Dent Sleep Med. 2020;7(4)
- Schwartz, David. “How Do Dentists Tackle the 54-Million-Pound Elephant Called Sleep Apnea?” Dental Sleep Practice, MedMark Media, 2021, dentalsleeppractice.com/how-do-dentists-tackle-the-54-million-pound-elephant-called-sleep-apnea/.
- Rosen IM, Kirsch DB, Carden KA, et al; American Academy of Sleep Medicine Board of Directors. Clinical use of a home sleep apnea test: an updated American Academy of Sleep Medicine position statement. J Clin Sleep Med. 2018 Dec 15;14(12):2075-7.
- Kapur VK, Auckley DH, Chowdhuri S, et al. Clinical practice guideline for diagnostic testing for adult obstructive sleep apnea: an American Academy of Sleep Medicine clinical practice guideline. J Clin Sleep Med. 2017 Mar 15;13(3):479-504.

 Dr. Jagdeep Bijwadia is board certified in internal medicine, pulmonary and sleep medicine. He is founder and CEO of a national sleep telemedicine practice (Sleepmedrx) serving all 50 US states. He also serves as Chief medical officer for Whole You. He currently holds a faculty position as Assistant Professor in the Department of Pulmonary Critical Care and Sleep Medicine at the University of Minnesota and has a private practice in Saint Paul, Minnesota. Dr. Bijwadia has been named top doc by the Minneapolis magazine as well as US News and World Report. He served as president for the Minnesota Sleep Society from 2016 to 2018 and is active in promoting sleep health in Minnesota. He also has an MBA from the University of St. Thomas in Minneapolis.
Dr. Jagdeep Bijwadia is board certified in internal medicine, pulmonary and sleep medicine. He is founder and CEO of a national sleep telemedicine practice (Sleepmedrx) serving all 50 US states. He also serves as Chief medical officer for Whole You. He currently holds a faculty position as Assistant Professor in the Department of Pulmonary Critical Care and Sleep Medicine at the University of Minnesota and has a private practice in Saint Paul, Minnesota. Dr. Bijwadia has been named top doc by the Minneapolis magazine as well as US News and World Report. He served as president for the Minnesota Sleep Society from 2016 to 2018 and is active in promoting sleep health in Minnesota. He also has an MBA from the University of St. Thomas in Minneapolis. Dr. Gregory Manning earned his Bachelor of Science in microbiology at Weber State University in Ogden, UT and his Doctor of Dental Surgery from The Ohio State University in 2006. He has been practicing dentistry in the Phoenix-area since 2008. Dr. Manning vigorously pursues continuing education in dental technology and sleep apnea treatment. He lectures extensively on these topics. He is a member of the American Dental Association, the Arizona Dental Association, the American Academy of Dental Sleep Medicine and is a diplomate of the American Sleep and Breathing Academy.
Dr. Gregory Manning earned his Bachelor of Science in microbiology at Weber State University in Ogden, UT and his Doctor of Dental Surgery from The Ohio State University in 2006. He has been practicing dentistry in the Phoenix-area since 2008. Dr. Manning vigorously pursues continuing education in dental technology and sleep apnea treatment. He lectures extensively on these topics. He is a member of the American Dental Association, the Arizona Dental Association, the American Academy of Dental Sleep Medicine and is a diplomate of the American Sleep and Breathing Academy.