Solving this Patient’s Dilemma
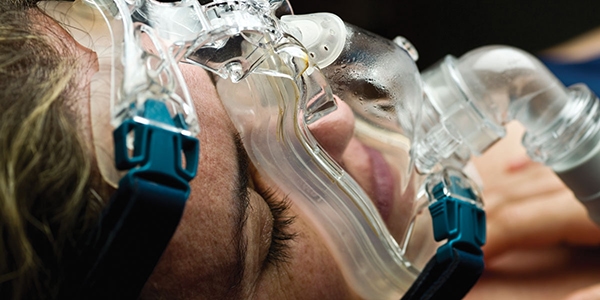
This is an interesting case where the patient was allergic to the silicone in the soft liner that is the interface of the CPAP mask to the face and also allergic to the neoprene straps of the CPAP mask. This middle aged woman has been trying to use the CPAP for 8 years off and on. She states that she cannot tolerate CPAP due to “allergy to neoprene,” which makes her face and nose red and itchy every morning (upon testing it was determined that it was actually the silicone as well that was the source of the allergic response). Since all CPAP masks use silicone, her options were very limited. This case will demonstrate that a Dentist trained in Combination Therapy can give people like this more options because the materials used in fabrication of custom masks do not include silicone. Combination Therapy (CBT) is combining CPAP (continuous positive airway pressure) therapy and OAT (oral appliance therapy) to resolve Obstructive Sleep Apnea (OSA).
Chief Complaint
A 56 year old woman with a body mass index (BMI) of 26 presents with intolerance to CPAP mask. She has a rare genetic craniofacial disorder called Treacher Collins Syndrome, which in her case results in an under developed zygoma and mandible (a challenge for a CPAP mask fit). Her chief sleep complaint is fatigue with falling asleep at inappropriate times. Her Epworth Sleepiness Scale (ESS) is 16 with the CPAP machine. She had a recent split night PSG with an AHI of 86, PSO2 87% (moderate OSA, but extremely fragmented sleep). CPAP with nasal pillow was started with a setting of 8cm H20. But she states that she cannot tolerate the nasal pillow due to allergy to the material, which makes her face and nose red and itchy every morning (just like the mask did in the past). She wears it for a few days and then has to stop for a week to allow the redness to subside while she deals with the extreme fatigue.
Clinical Findings
Her blood pressure was 142/84 and her neck circumference was 15 inches. Palpation of the TM Joints revealed tenderness in both joints indicating capsulitis of the joints. The temporalis, deep masseter, and lateral pterygoid muscles were tender on both sides. Her mandibular range of motion (ROM) was only 28mm with pain. Because of her Treacher Collins Syndrome, she has a significant retrognathic skeletal relationship. Oral examination indicated that she has many signs and symptoms of clenching at night including scalloping of the tongue, linea alba, high vaulted palate, narrow dental arches, mandibular tori and significant wear facets on her teeth. She also has an anterior open bite secondary to her retrognathia, but also because of her tongue thrust at night. Because of the degenerative changes in the left condyle, her mandibular midline was 1mm left of facial midline. The cone-beam x-ray (i-CAT) indicated that she has concha bullosa of the left middle turbinate and slight degenerative changes in the left TM joint (with a subcondyral cyst). And as expected based on physical exam, she also has an extremely small airway.
It was obvious by her continuing fatigue and nocturnal clenching/bruxing that the CPAP machine that she has been using has not adequately resolved her OSA. She still had many compensatory mechanisms in place because the airway was not stable. These compensatory mechanisms include clenching and bruxing at night, which causes fragmentation of her sleep and the fatigue that she is dealing with. The allergies that she had from the silicone may be contributory to her fragmented sleep and the concha bullosa may have restricted nasal airflow. With her significant number of arousals, hypoxemia, and cardiovascular concerns, it was my judgment to proceed directly to combination therapy to stabilize her airway to see if we can demonstrate the resolution of all her symptoms before we consider mandibular advancement splint (MAS). When the MAS is considered in her case, there will be many challenges. First she has arthritic TM joints (especially the left) with pain. Then she has retrognathia which will make advancing the mandible to a significant degree a challenge. The open bite is also challenging as the MAS has a tendency to make that situation worse. As a result, overall the fact that she has TMJ symptoms, it was my judgment that entering right into the mandibular advancement splint would aggravate her TMJ condition and basically make her overall sleep worse. So the rational to move right into Combination Therapy (CBT) is based on first demonstrating resolution of symptoms (mainly fatigue) with a stable airway. If the airway is stable, and the sleep structure restored to normal and the fatigue is gone, then a transition to a MAS can be attempted with the best possible outcome. But if the airway is stable and she still has fatigue, then other reasons for the fragmented sleep will have to be explored.
Treatment Outcome
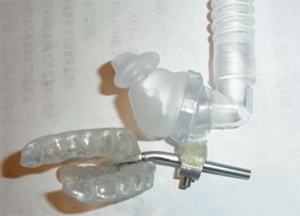
A TAP-PAP™ CS (with nasal pillows) was attempted first to see if she could tolerate the nasal pillows. This device is designed to attach nasal pillows to a post that is screwed directly onto a TAP3™ mechanism. Then the CPAP hose is clipped into the nasal pillows. The result is that there are no straps and nothing touching her face except the nasal pillows in her nose. There is no movement and the mandible is stable with the mouth closed with the TAP3™ upper and lower glued together with Thermocryle™. Even with this set up, she had leakage of air through her oral cavity at night and she explains that the nasal pillows (which came from the Fischer Paykel Opus™ mask) also cause redness around her nose (they were made of silicone). This indicated to me that she not only had a neoprene problem, but also an allergy to silicone. A piece of neoprene, silicone and acrylic was taped to her arm for three days to determine which material would give her an allergic response. The result was that she had a wheal and flare allergic skin response to the silicone and the neoprene, but not the Biocryl™ acrylic (Great Lakes Orthodontics). Therefore, face impression was taken for a TAP-PAP™ CM (Custom Mask), to be made from Biocryl. The TAP-PAP® CM was fabricated for her. Her mandible was stable with a 3 mm protrusion to augment the CPAP. There was no leakage and she was able to take it off and on with no struggles. It was very quiet and stable. She explained that she has had the best night sleep that she has ever had. She was sent to her daughter who is a local sleep physician for a re-titration of her CPAP machine. The pressures were reduced to 7 cm H20. As a result her ROM increased, her TM Joint pain resolved and her fatigue levels were significantly reduced (ESS 9), although not totally. She wants to remain in the Custom Mask for at least a year before considering a MAS.

“Thank you seems so inadequate for the gift of sleep that you have given me. I would have never thought I would have seen such the differences I have. Initially, my goal was just get rid of the neoprene headgear, I never expected it would also be the great improvement in the quality of sleep that I would experience. I cannot remember when I ever (and I do mean ever) woke up feeling refreshed like I had a great night sleep until the introduction of the TAP-PAP into my life. Again, thank you.”
Summary
As a Dentist who treats conditions related to Sleep Disordered Breathing (SDB), there are many aspects of the profession that can be applied to treatment options. The knowledge of materials that can be used to treat these conditions and conditions that effect the facial structures are well known to a Dentist. This case challenged both aspects of care. The joy of treating these SDB conditions is realized when the lives of our patients are improved and the SDB condition is resolved.





